While root canal therapy is a cornerstone of modern restorative dentistry, boasting success rates as high as 95%, clinical challenges can occasionally lead to treatment failure.
Root canal treatment is designed to save a natural tooth by removing infection from its internal structure. However, when a tooth does not heal as expected or when pain recurs months or years later, it is often due to a "re-infection" rather than a failure of the procedure itself.
Why Do Root Canals Fail?
Experts identify several key factors that can compromise the longevity of the treatment:
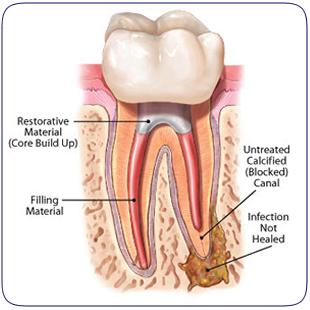
- Complex Anatomy: The internal structure of a tooth is a web of microscopic canals. If a particularly small or "hidden" canal is missed during the initial cleaning, bacteria can remain trapped and eventually cause a new infection.
- Restoration Delay: After a root canal, the tooth is often brittle and requires a crown. If the permanent restoration is delayed or if the seal breaks, bacteria from the mouth can leak back into the tooth, a process known as coronal microleakage.
- Persistent Bacteria: Certain hardy strains of bacteria can occasionally survive the disinfection process, requiring specialized secondary treatments or endodontic surgery.
- Structural Fractures: In some cases, a tooth may develop a microscopic vertical crack that is undetectable during the initial procedure but allows bacteria to re-enter over time.
Patient Indicators for Follow-up
Patients who have undergone root canal therapy should remain vigilant for signs of "post-treatment disease." Early intervention often allows for successful retreatment, saving the tooth from extraction. Key symptoms include:
- Return of Sensitivity: Especially from pressure or percussion.
- Swelling: Any inflammation in the gums near the treated tooth.
- The "Pimple" Effect: The appearance of a small bump on the gum line, indicating a drainage point for underlying infection.
Shelan Shwan Abdulrahman
Assistant Lecturer, Faculty of Dentistry
Qaiwan International University