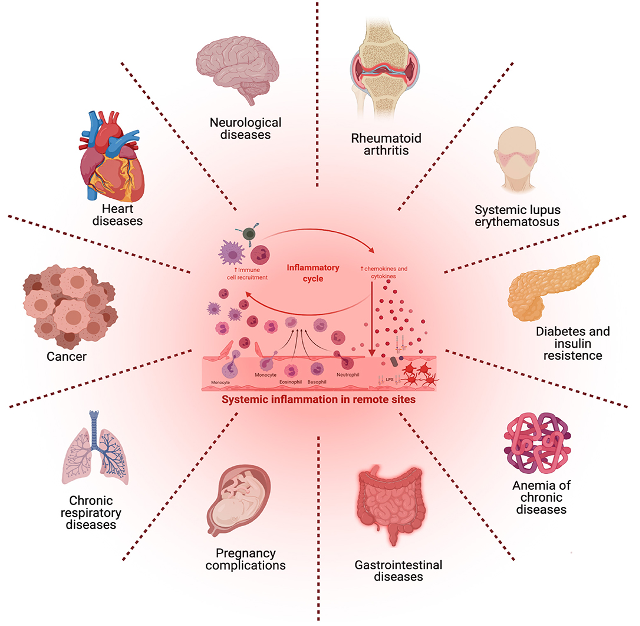
The relationship between periodontal disease and systemic diseases
Emerging evidence suggests that periodontal inflammation may contribute to the pathogenesis and progression of various systemic conditions. Chronic periodontal infection can lead to elevated levels of inflammatory mediat…
Read More